According to new analysis by Oliver Wyman, 2016 was the year of payer-provider partnerships – and more of the same can be expected in 2017.
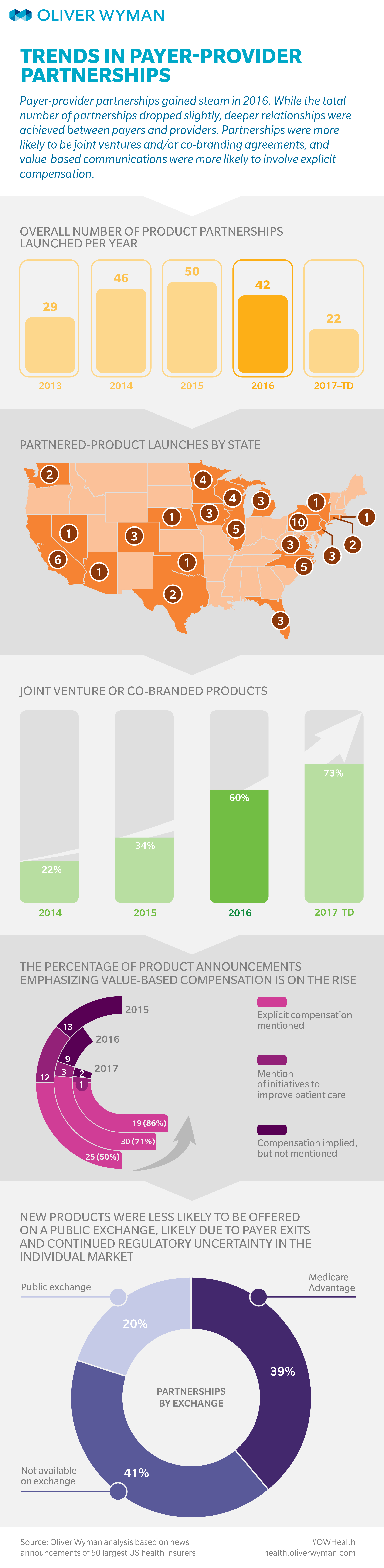
In 2016, new product launches were announced at a steady clip and there was greater emphasis on longer-term collaboration through joint ventures and co-branded relationships, where quality, value, and joint efforts to control total cost of care are as important as traditional rate-card negotiations (see our infographic below).
Although uncertainty around public exchanges and the resulting payer exits led to a slight decline in the total number of new product launches, there was a marked growth in off-exchange products, particularly Medicare Advantage. There also was a shift away from undifferentiated, fee-for-service narrow networks, with a larger portion of products utilizing provider co-branding and explicitly mentioning value based compensation models in launch announcements.
The partnerships themselves also tended to be deeper, with a much higher prevalence of joint ventures. For example, Banner Health announced a joint venture with Aetna to launch a new insurance company (Banner | Aetna) as the next step in their existing Aetna Whole Health relationship. The new venture promises to deliver better outcomes and provide members with a seamless experience across payer and provider.
Beyond deepening existing partnerships, many players also entered into new partnerships. For example, Aetna’s Whole Health program continued to launch new products with local providers in several markets. The Blues were also active in launching provider-partnered products. Highmark Blue Shield unveiled a new tiered-benefit plan Pennsylvania, known as Alliance Flex Blue, with Penn State Milton S. Hershey Medical Center and PinnacleHealth; and Blue Cross Blue Shield of Illinois launched BlueCare Direct with Advocate Health Care targeting cost-sensitive consumers.
Payer-provider partnered products continue to offer an alternative pathway to value, creating the opportunity to build a collaborative relationship that extends beyond the limitations of traditional narrow networks and open the door to a host of unique opportunities to improve health status and quality of care for consumers.
The below infographic highlights key trends in payer-provider partnerships.